People-Centered Care Working Definition
People-centredness is an approach to providing the continuum of care that incorporates the needs, values, and preferences of individuals in the context of their communities. It promotes respectful, empathetic, dignified and collaborative relationships between persons and all those who contribute to healthcare, ensuring that care is not only clinically effective but also emotionally supportive and trustworthy. People-centred care is a foundation for implementing the right to health and to achieving wellbeing outcomes, and a good care experience. It is achievable when there is a shift to collaborative and co-created health and care systems.
People-Centered Care Antecedents, and Consequences
Antecedents
Conditions needed for people-centred healthcare to be enacted
- Health system: Integrated health systems that are adequately resourced, managed and organized around people's' needs, cultures and contexts, and are underpinned by a commitment to staff training, education, and positive safe working conditions.
Societal factors: Social governance and community structures, cultures and norms that promote equity, social participation, accountability and culturally-safe practices, to address structural and social determinants of health and well-being
Characteristics
The defining features of people-centred care that distinguishes it from other modes of healthcare delivery
Clinically effective care that ensures technical, evidence-based quality of prevention, promotion, diagnosis, treatment, rehabilitation, and palliation across the continuum of care
Care that empowers individuals and communities to meaningfully participate in health promoting behaviours, individual care, and service/system design
Emotionally-responsive and affirming care mediated through respectful, trustworthy, compassionate, collaborative relationships with providers, families, and the care team
Holistic and inclusive care that promotes wellness, is safe, responds to diverse personal and community preferences, culture,s and contexts, including the SDoH, and is rooted in lived experiences
Care that is easy to access, affordable, and which maximises continuity of experience, as well as health system efficiency, utilisation, and effectiveness
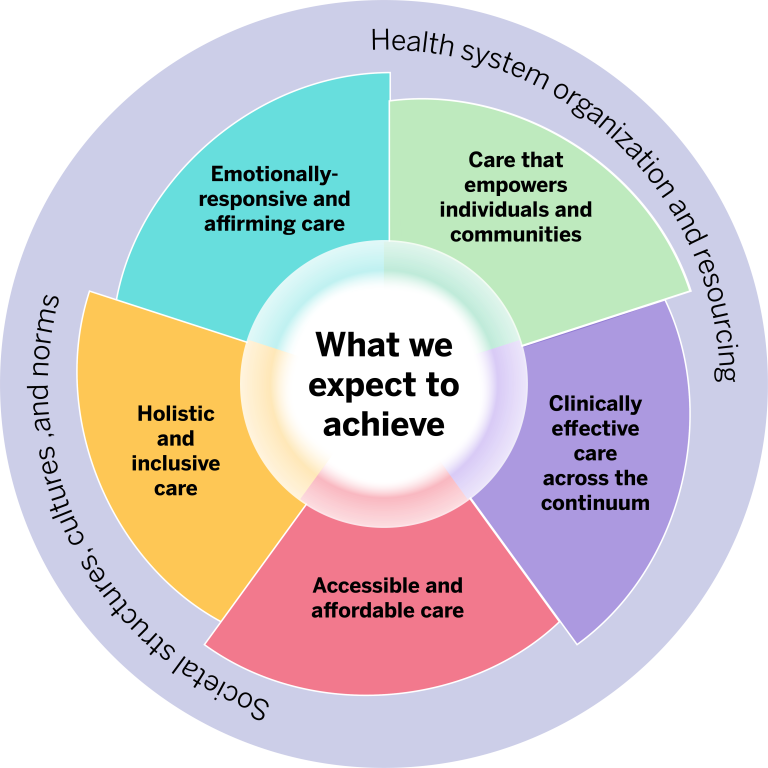
Consequences
What we expect to achieve when people-centered care is enacted
Personal Agency & Self‑Efficacy: Growth in individuals' perceived control and capability to influence their health and care
Engagement in Care: Active participation in care processes and decisions, leading to more consistent health behaviours
Access & Continuity of Care: Improved ability to obtain services and maintain ongoing, coordinated care over time
Wellbeing: Improved physical, psychological, and social outcomes through affirming and trusting relationships
Cultural Safety & Equity: Care environments and practices that are respectful, responsive, and safe for service users and service providers
- Collective Empowerment: Communities exercising decision-making authority and influence over health priorities and services through inclusive governance.